Health at a Glance
Archived Content
Information identified as archived is provided for reference, research or recordkeeping purposes. It is not subject to the Government of Canada Web Standards and has not been altered or updated since it was archived. Please "contact us" to request a format other than those available.
Mental health of the Canadian Armed Forces
Statistics Canada Catalogue no. 82-624-X
by Caryn Pearson, Mark Zamorski and Teresa Janz
- Highlights
- Lifetime rates among Regular Force members
- Depression was the most common disorder in the past 12 months
- Mental disorders higher for women; alcohol abuse or dependence higher for men
- Mental disorders were higher among deployed Regular Force members
- What has changed since 2002?
- Comparing data from 2002 with 2013
- How does the mental health of Regular Force members and Canadians compare?
- Comparing content of the 2012 Canadian Community Health Survey – Mental Health and the 2013 Canadian Forces Mental Health Survey
- Summary
- What you need to know about this study
- Notes
- Related material for this article
Highlights
- In 2013, about 1 in 6 full-time Regular Force members of the Canadian Armed Forces reported symptoms of at least one of the following disorders: major depressive episode, panic disorder, post-traumatic stress disorder, generalized anxiety disorder, and alcohol abuse or dependence.
- Depression was the most common disorder with 8.0% of Regular Force members reporting symptoms in the past 12 months.
- The 12-month rates for post-traumatic stress disorder and panic disorder were twice as high among Regular Force members who had been deployed in support of the mission in Afghanistan compared to those who had not.
- Between 2002 and 2013 the rate of depression among Regular Force members has not changed, while the rates of post-traumatic stress disorder and panic disorder increased.
- Regular Force members had higher rates of depression and generalized anxiety disorder than the general Canadian population.
Understanding the mental health of the Canadian Armed Forces has important implications for those who have disorders and for military organizations. At the individual level, mental disorders are commonly associated with distress or disability, behavioural or psychological dysfunction, pain, and sometimes death.Note 1 For the military, these conditions have been identified as the leading causes of reduced productivity, absenteeism, and turnover.Note 2, Note 3
Military populations are at potential risk of mental health issues because their job can involve exposure to trauma, separation from family, frequent moves and stressful living conditions.Note 4 Exposure to traumatic events during combat and peacekeeping missions has been associated with mental disorders in military personnel.Note 5 For example, previous research found that among members of the Canadian Armed Forces who were deployed in support of the Afghanistan mission between 2001 and 2008, about 13.5% had been clinically diagnosed with a mental disorder that could be linked to their involvement in the Afghanistan mission.Note 6
This article describes results from the 2013 Canadian Forces Mental Health Survey (CFMHS). The survey collected information on five selected mental disorders from full-time regular members of the Canadian Forces, and only reservists who had been deployed in support of the mission in Afghanistan. This article highlights both lifetime and 12-month rates of five selected disorders for Regular Force members. Lifetime rates reflect those who had met the criteria for a disorder at some point in their life. In contrast, the 12-month rates provide information on recent cases. The 12-month rates are examined by sex and deployment history, and they are compared with both the 2002 rates and those from the general Canadian population.
This article refers to two types of Canadian Armed Forces members:
- Regular Force members serve as full-time members of the Canadian Armed Forces. When required, deploymentNote 7 within Canada or overseas is mandatory. Deployments include responding to national disasters, peacekeeping, or involvement in combat and peace support missions, such as the Afghanistan mission.Note 8 About 45% of Regular Force members included in this survey had been deployed in support of the mission in Afghanistan.
- Reserve Force members (reservists) largely serve part-time in the Canadian Armed Forces. Their main role is to support the Regular Force at home and abroad. Reservists may be asked to serve full-time as part of a mission overseas; however, their participation is effectively voluntary,Note 9 and most reservists never deploy. Consistent with the objectives of this survey, only Reserve Force members deployed in support of the mission in Afghanistan were interviewed.
Lifetime rates among Regular Force members
In 2013, about one-half of Regular Force members (48.4%) met the criteria for at least one of the five selected mental or alcohol disorders at some point in their lives (Table 1).
Alcohol abuse or dependence was the most common disorder with one-third of Regular Force members (31.9%) meeting the criteria in their lifetime. This finding parallels the general Canadian population, where in 2012, alcohol abuse or dependence was also the most common disorder over the lifetime.Note 10
Alcohol abuse (24.1%) was more commonly reported than alcohol dependence (7.8%) among Regular Force members, just as it was in the general Canadian population (data not shown).Note 11 Past alcohol abuse or dependence made the largest contribution to the overall rate of lifetime disorders in both the Regular Force and Canadian populations.
Depression was the second most common disorder experienced over the lifetime, followed by post-traumatic stress disorder and generalized anxiety disorder. About the same proportion of Regular Force members reported symptoms of generalized anxiety disorder (12.1%) and post-traumatic stress disorder (11.1%) in their lifetime.
Symptoms of panic disorder, characterized by unexpected recurrent attacks of intense fear and anxiety in the absence of real danger, were reported as having occurred by 5.8% of Regular Force members at some point in their lifetime.
| Lifetime | 12-month | |
|---|---|---|
| percentage | ||
| Any selected mental or alcohol disorderNote 1 | 48.4 | 16.5 |
| Depression | 15.7 | 8.0 |
| Generalized anxiety disorder | 12.1 | 4.7 |
| Post-traumatic stress disorder | 11.1 | 5.3 |
| Panic disorder | 5.8 | 3.4 |
| Alcohol abuse or dependenceNote 2 | 31.9 | 4.5 |
| Alcohol abuse | 24.1 | 2.5 |
| Alcohol dependence | 7.8 | 2.0 |
|
Source: Statistics Canada, Canadian Forces Mental Health Survey, 2013. |
||
Depression was the most common disorder in the past 12 months
Focusing on 12 month rates for the remainder of the article, overall, 1 in 6 Regular Force members (16.5%) identified symptoms of at least one of the following five mental or alcohol disorders: major depressive episode, panic disorder, post-traumatic stress disorder, generalized anxiety disorder, and alcohol abuse or dependence (Table 1).
Depression was the most common of these disorders, with 8.0% of Regular Force members reporting symptoms over the past 12 months. Post-traumatic stress disorder and generalized anxiety disorder were the next most common mental disorders, followed by panic disorder. About the same proportion of Regular Force members reported symptoms of post-traumatic stress disorder (5.3%) and generalized anxiety disorder (4.7%).
Mental disorders higher for women; alcohol abuse or dependence higher for men
In 2013, among Regular Force members, rates of depression, generalized anxiety disorder and post-traumatic stress disorder were higher for women than for men, while alcohol abuse or dependence were higher for men (Chart 1).

The percentage of female Regular Force members who reported symptoms of post-traumatic stress disorder in the past 12 months was almost double (8.8%) that of their male counterparts (4.7%). On the other hand, the rate of alcohol abuse or dependence among males was almost double (4.8%) that of females (2.3%Note 12). About the same percentage of male and female Regular Force members met the criteria for panic disorder in the past 12 months.
These findings of higher rates of depression and anxiety disorders among women, and higher rates of alcohol abuse or dependence in men, are consistent with past research on Canadian Forces personnel,Note 13 the general Canadian population,Note 14 and the general population of many other countries.Note 15
Mental disorders were higher among deployed Regular Force members
In 2013, about 45% of Regular Force members had deployed since 2001 in support of the mission in Afghanistan. This includes deployments in Afghanistan as well as elsewhere in southwest Asia.
Regular Force members who had been deployed in support of the mission in Afghanistan had higher rates of mental disorders than their non-deployed counterparts (Chart 2).

The rates of post-traumatic stress disorder and panic disorder were twice as high among deployed Regular Force members compared with those who were not deployed. In contrast, non-deployed Regular Force members (5.4%) were more likely to report symptoms of alcohol abuse or dependence than their deployed counterparts (3.4%).
Reserve Force members who had been deployed in support of the mission in Afghanistan had similar rates of mental disorders compared with deployed Regular Force members, except for alcohol related disorders, where Reserve Force members had higher rates (data not shown). The Reserve Force population is younger with more males than the Regular Forces, which may contribute to the higher rates of alcohol related disorders among reservists.Note 16
These findings are similar to past research that found participation in combat and peacekeeping missions was associated with mental disorders among military personnel.Note 17
What has changed since 2002?
In 2002 and 2013, the 12-month rates for depression were about the same at 8.0% among Regular Force members.Note 18 However, the rates for panic disorder and post-traumatic stress disorder were both higher in 2013 (Chart 3). Post-traumatic stress disorder was twice as high in 2013 (5.3%) compared with 2002 (2.8%).

Some of these differences in the rates of mental disorders over time can be understood in a context of changes since 2002. That is, more than 40,000 Canadian military personnel were deployed in combat and peace support missions in Afghanistan and 158 of them lost their lives.Note 19, Note 20 Differences in the rates over time may also be related to changes in mental health programs designed to support Canadian Armed Forces personnel.Note 21
Comparing data from 2002 with 2013
In order to look at changes in mental health over time, two surveys were used: (1) the 2013 Canadian Forces Mental Health Survey (CFMHS) and (2) the 2002 Canadian Community Health Survey–Mental Health and Well-being –Canadian Forces (CCHS–CF). Some disorders from these surveys are comparable and some are not. This is because of differences between the two surveys in the selection of disorders, the survey questions, the sample and the populations they represent.
The rates for Reserve Force members for 2002 and 2013 cannot be compared across the two surveys because the criteria for selecting Reservists differed for each survey. In 2013, only those deployed in support of the mission in Afghanistan were surveyed. In 2002, on the other hand, Reserve Force members who were not deployed, as well as those who were deployed, were interviewed for the survey.
The two surveys measured disorders according to criteria from the World Health Organization Composite International Diagnostic Interview (WHO – CIDI), which has been revised since 2002. As a result of the updates, generalized anxiety disorder and alcohol abuse have changed in the way they are assessed and cannot be compared.
The disorders that can be compared using 2002 and 2013 data are depression, post-traumatic stress disorder and panic disorder.
How does the mental health of Regular Force members and Canadians compare?
In general, the population of the Regular Forces is younger and there are more males than the general Canadian population. In order to compare rates of disorders between these two populations, the general Canadian population was age and sex standardized to the Regular Force population in 2013 to take the age and sex differences into account.
Age and sex standardized estimates are used in this article to adjust the age and sex distribution of the Canadian population to reflect a similar distribution of the Regular Force population. The estimates calculated for the standardized population are a measure of what the rate would be if both populations had the same age and sex structure. In this case, the Canadian rates were changed to reflect a similar proportion of males and younger people found in the Regular Forces. Thus, the Canadian rates have been created to provide a context for comparison.
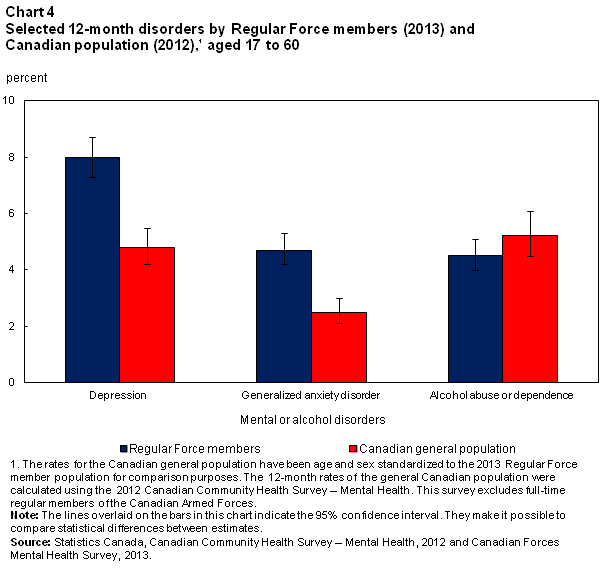
Compared with the general Canadian population, rates of mental disorders were higher among Regular Force members. The percentage of Regular Force members who reported symptoms of depression and generalized anxiety disorder in 2013 was almost double that of the general Canadian population in 2012 (Chart 4). In 2002, Regular Force members also had higher rates of depression and panic disorder than the Canadian population.Note 22
Approximately the same percentage of Regular Force members and the general Canadian population met the criteria for alcohol abuse or dependence in the 12 months prior to the survey. Close to 5% of Regular Force members and Canadians reported symptoms consistent with alcohol abuse or dependence.
Comparing content of the 2012 Canadian Community Health Survey – Mental Health and the 2013 Canadian Forces Mental Health Survey
The disorders that can be compared from both the 2013 Canadian Forces Mental Health Survey and the 2012 Canadian Community Health Survey – Mental Health are: depression, generalized anxiety disorder and alcohol abuse or dependence. The two surveys do not measure post-traumatic stress disorder using the same criteria and, as a result, these rates are not comparable.
Summary
In the 12 months prior to the 2013 survey, about 1 in 6 (16.5%) Regular Force members reported symptoms consistent with at least one of the five selected mental disorders: major depressive episode, panic disorder, post-traumatic stress disorder, generalized anxiety disorder, and alcohol abuse or dependence. While male Regular Force members reported more symptoms of alcohol abuse or dependence, females reported more symptoms of depression, post-traumatic stress disorder and generalized anxiety disorder.
A larger percentage of Regular Force members who had deployed in support of the mission in Afghanistan reported symptoms of at least one of the five selected mental disorders (18.9%) in the past 12 months, compared with their non-deployed counterparts (14.6%).
Between 2002 and 2013, rates of depression among Regular Force members remained relatively stable at around 8%, while rates of panic disorder and post-traumatic stress disorder rose.
When compared with the Canadian population, a larger percentage of Regular Force members reported symptoms consistent with depression and generalized anxiety disorder, while about the same percentage met the criteria for alcohol abuse or dependence in both populations.
What you need to know about this study
The rates presented for various disorders may underestimate the extent of mental health issues in the Canadian Armed Forces. This is because the Canadian Forces Mental Health Survey 2013 (CFMHS) measured five selected disorders, meaning not all mental disorders were covered by the survey. This same limitation applies to all mental health surveys. The CFMHS collected information from full-time Regular Force members of the Canadian Armed Forces and only from those reservists who had been deployed in support of the mission in Afghanistan.
Mental or alcohol disorders
The CFMHS 2013 used the World Health Organization - Composite International Diagnostic Interview 3.0 (WHO-CIDI) to classify people as meeting the criteria for select disorders. Although this is not a clinical diagnosis, this standardized instrument is designed to assess disorders in population surveys according to the Diagnostic and Statistical Manual of Mental Disorders version IV (DSM-IV).
This paper analyzes five disorders (lifetime and 12-month):
1. Alcohol abuse or dependence:
- Alcohol Abuse is characterized by a pattern of recurrent alcohol use where at least one of the following occurs: failure to fulfill major roles at work, school or home, use in physically hazardous situations, recurrent alcohol-related problems, and continued use despite social or interpersonal problems caused or intensified by alcohol.
- Alcohol Dependence is when at least three of the following occur in the same 12-month period: increased tolerance, withdrawal, increased consumption, unsuccessful efforts to quit, a lot of time lost recovering or using, reduced activity, and continued use despite persistent physical or psychological problems caused or intensified by alcohol.
2. Depression (major depressive episode): is identified as a period of two weeks or more with persistent depressed mood or loss of interest in normal activities, as well as other symptoms including: decreased energy, changes in sleep and appetite, impaired concentration, feelings of hopelessness, or suicidal thoughts.
3. Generalized anxiety disorder: is identified by a pattern of frequent, persistent worry and excessive anxiety about several events or activities lasting at least six months along with other symptoms.Note 23
4. Panic disorder: is marked by recurrent, unexpected panic attacks, in the absence of real danger. These attacks are followed by at least one month of concern about having additional attacks or a change in behaviour related to the attacks.
- Panic attack: is characterized by an isolated period of intense fear often associated with feelings of imminent doom. During these attacks, physical symptoms, such as heart palpitations, shortness of breath, or sweating, develop abruptly and reach a peak within 10 minutes of the start of the attack.Note 24
5. Post-traumatic stress disorder: can occur after witnessing or experiencing a traumatic event involving actual or threatened death, serious injury or violent personal assault, such as sexual assault. The response to the event is marked by extreme fear and helplessness. Symptoms must persist for a minimum of one month and could include: repeated reliving of the event, disturbance of day-to-day activity, avoidance of stimuli associated with the event, and irritability, outbursts of anger, or sleeping difficulty.
Caryn Pearson and Teresa Janz are analysts with the Health Statistics Division. Mark Zamorski is a Senior Medical Epidemiologist, Directorate of Mental Health, Canadian Forces Health Services Group, National Defence.
The authors wish to thank Jennifer Ali, Barbara Sérandour, and Melanie Hoover for their contributions to this article.
Notes
Related material for this article
Additional information
- For more statistics and analysis on the health of Canadians and the health care system, visit the Health in Canada module. This module is accessible from our website, under Features.
Related Articles
Data sources
Bibliographic references
- Date modified:
